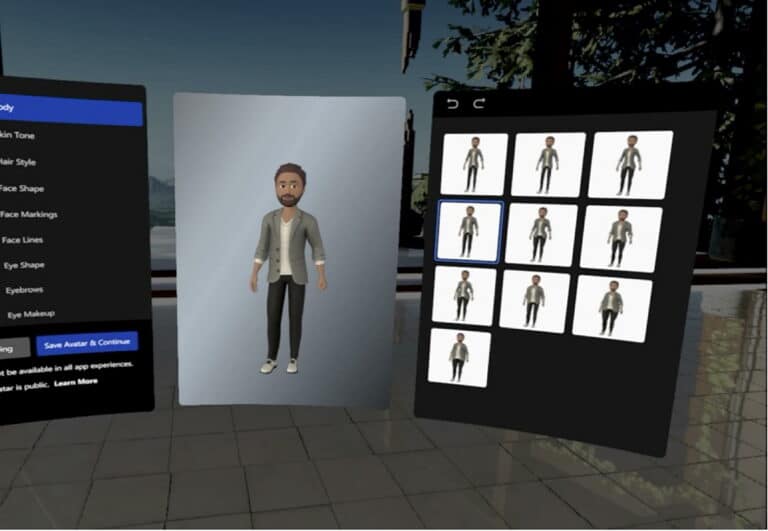
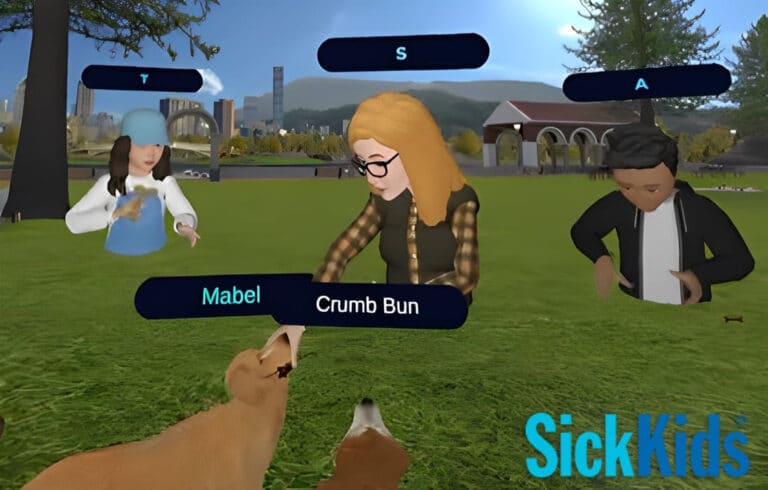
In person group-based intensive outpatient programs (IOPs) have shown promising results for adults with serious mental illnesses. At the start of pandemic, these IOPs were forced to meet remotely through video-based telemental health (TMH) platforms presenting an opportunity to better understand the benefits and drawbacks of online group therapy.
A recent study from the Mayo Clinic focused on TMH group-based IOPs, providing insight into the effectiveness of and overall patient satisfaction with this type of treatment. Researchers interviewed 76 patients with diagnosed serious mental illness (SMI) who participated in an online video group based IOP.
Researchers gathered their data using a 17-item questionnaire covering 3 areas: “IOP TMH satisfaction, future recommendations, and video technology challenges.” According to the feedback they received, “the majority of patients reported high satisfaction, comfort, appropriateness, relevance, and compatibility” of the TMH service, 92.5% of them reporting “that they would recommend this service format to a friend or family member.” Most patients were glad to have the option for treatment during COVID, one even commenting that it was “just like being in a room full of people” and it “saved [their] life.”
Despite the fact that group telehealth was viewed favorably overall, there were reported challenges during the program. Slow internet connection, poor video camera quality, login problems, and accidental removal from the session were the most highly reported of these challenges. One of the participants noted that the Zoom meetings didn’t feel as welcoming, and “’there couldn’t really be a discussion [as if they were] sitting in the same room.’” Another wanted “more collaboration among the patients.”
Other participants wished they had used “’more of the Zoom features such as the whiteboard,’” or recommended “’some tabs to find things [easier].”’ There seemed to be a large disconnect with the learning materials in general. Patients suggested that administrators work on “improving the structure of the binder.” Some of the patients didn’t like the program at all because of the video format and desired something more immersive and interactive.
Though the study affirms that remote group therapy was well received in general, there were clear deficiencies noted. Virtual Reality (VR) for group therapy addresses many of these concerns and offers other benefits not possible through video-based TMH.
“poor video camera quality”
Instead of sitting in front of a camera, group therapy in VR allows participants to sit, lie down, or walk around in their physical environment. More importantly, everyone is portrayed as a personalized avatar which creates a consistent visual and auditory experience regardless of room lighting or camera or microphone quality. The need not to be on camera also takes away judgement of physical appearance and removes outside environmental distractions.
“there couldn’t really be a discussion [as if they were] sitting in the same room”
Unlike group video sessions in which everyone is arranged on a flat grid, VR sessions are held in a shared, 3D environment. This means that participants who look around the room will see one another from the same perspective as they would in the physical world. For example, to see the person who is slightly out of view to my left, I would turn my head in that direction and they would appear in front of me. Since everyone is sitting in a shared environment, they also see the same things as one another creating a stronger sense of connection.
“more of the Zoom features such as the whiteboard”
Just as with Zoom, VR offers many tools for collaboration and instruction including white boards, sticky notes, and media presenting. But VR also provides the ability to manipulate and pass 3D objects, draw in space, and watch fully enveloping 360 video.
“more collaboration among the patients”
True collaboration in Zoom in a challenge because we as humans collaborate in 3D space. VR provides the ability to collaborate in ways not possible on Zoom whether that means team building exercises, collaborative role play with avatars, or simple games that bring people together.
“improving the structure of the binder”
A foundation of many IOPs is the presentation of a structured curriculum which is outlined in binders provided to patients who follow along during each session. With limited space to view and absorb material, video sessions present a challenge when it comes to conveying this material. With VR, patients can reference their binder from their own personal screen while also collectively viewing material on the therapists screen(s). Navigating between materials and interacting with them is much more intuitive as it mimics the 3D world.
VR also provides benefits not identified above. For example, avatars allow for exploration of identity, role play activities and anonymity if desired. All or parts of sessions can be recorded and played back in 3D allowing for analysis and reflection from the group. And analytics such as time spent speaking and direction of gaze provide insights for both patient and therapist.
Foretell Reality is an avatar-based, multi-participant virtual reality platform specifically designed for group therapy and support. Please click here for more information or to schedule a demo.